New research suggests that vitamin D supplements can reshape how the immune system responds to gut bacteria in patients with inflammatory bowel disease, potentially nudging the body toward a more protective, less inflammatory state. The findings offer early clues toward therapies that restore immune tolerance rather than simply suppress symptoms.
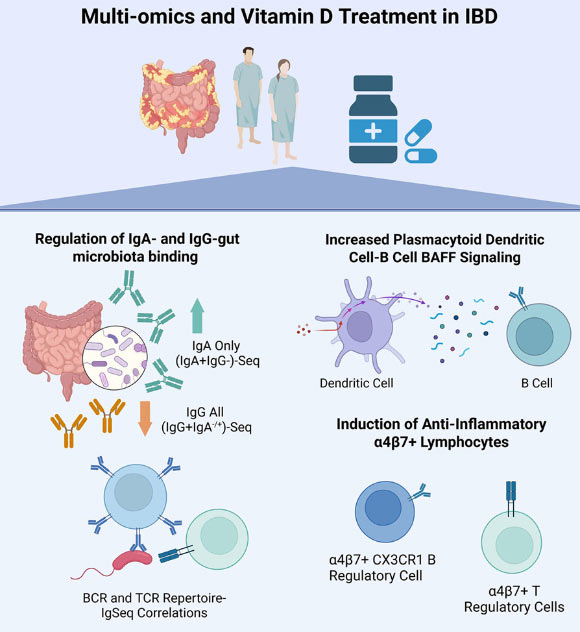
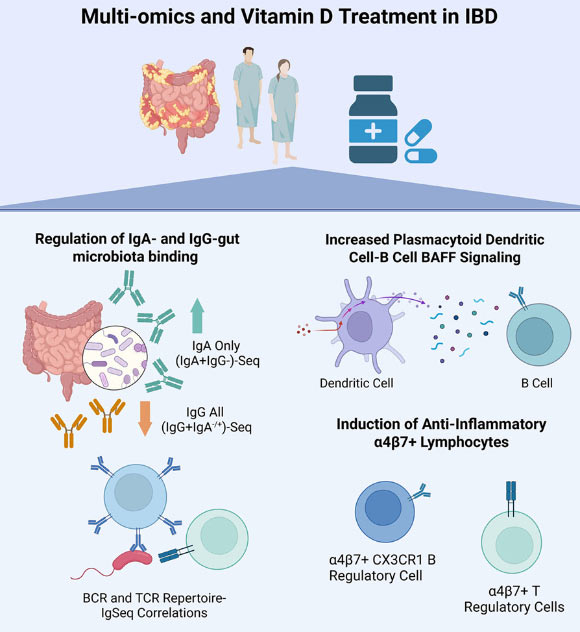
Gubatan et al. demonstrate that vitamin D promotes immune tolerance to gut microbiota in patients with inflammatory bowel disease. Image credit: Gubatan et al., doi: 10.1016/j.xcrm.2026.102703.
Inflammatory bowel disease (IBD), which includes ulcerative colitis and Crohn disease, is a chronic inflammatory disorder of the gastrointestinal tract that is thought to arise from a complex interplay between host genetic predisposition1 and environmental triggers.
Loss of immune tolerance to commensal gut bacteria has been recognized to play a pivotal role in the pathogenesis of IBD.
Current therapeutic strategies in IBD have focused mainly on targeting dysregulated immune responses without directly addressing gut microbiome crosstalk with intestinal immunity.
Understanding the mechanisms that regulate host immune-microbe interactions and developing ways to restore immune tolerance to gut microbiota could lead to therapeutic strategies to treat or prevent IBD.
“This study suggests vitamin D may help rebalance how the immune system sees gut bacteria,” said Dr. John Mark Gubatan, a gastroenterologist at Mayo Clinic.
“That’s an important step toward understanding how we might restore immune tolerance in IBD.”
In the new study, the researchers evaluated 48 people with IBD who had low vitamin D levels.
Participants received weekly vitamin D supplements for 12 weeks. Blood and stool samples collected before and after treatment were analyzed using advanced sequencing to map interactions between immune responses and the gut microbiome.
Vitamin D supplementation was associated with increased levels of immunoglobulin A (IgA), which is typically linked to protective immune responses, and decreased levels of immunoglobulin G (IgG), more often associated with inflammation.
The scientists also observed changes in immune signaling pathways and increased activity of regulatory immune cells that help control inflammation.
Together, these findings suggest vitamin D may help promote a more balanced, protective immune response to the gut microbiome.
Vitamin D supplementation was also associated with improvements in disease activity scores and a stool-based marker of inflammation.
However, the authors emphasize the study was small and not designed to establish cause and effect.
“We saw encouraging signals, but this was not a randomized trial,” Dr. Gubatan said.
“These findings need to be confirmed in larger, controlled studies.”
The researchers caution that patients should not change their vitamin D use without medical guidance.
“Vitamin D is widely available, but dosing needs to be individualized, especially in patients with chronic inflammation. Patients should work with their healthcare team,” Dr. Gubatan concluded.
The study was published in the journal Cell Reports Medicine.
_____
John Gubatan et al. Multi-omics reveal vitamin D regulation of immune-gut microbiome interactions and tolerogenic pathways in inflammatory bowel disease. Cell Reports Medicine, published online March 26, 2026; doi: 10.1016/j.xcrm.2026.102703